PATCH
Platelet transfusion versus standard care after acute stroke due to spontaneous cerebral haemorrhage associated with antiplatelet therapy (PATCH): a randomised, open-label, phase 3 trial
Baharoglu. Lancet 2016; 387:2605–2613. doi:10.1016/S0140-6736(16)30392-0
Clinical Question
- In patients with acute intracerebral haemorrhage (ICH), associated with antiplatelet therapy, does platelet transfusion compared with standard care reduce death or dependence?
Design
- Randomised controlled trial
- Web-based randomisation system
- Biased coin randomisation
- Clinicians and patients non-blinded
- Primary outcome assessed by blinded neurologist or research nurse performing either structured telephone interview or face to face consultation
- Primary outcome modified from that specified in trial protocol. Modification occurred prior to unmasking the trial database and without knowledge of outcome data.
- Intention to treat analysis
- 91% power to detect a common odds ratio (OR) of 0.43 in an ordinal logistic regression analysis for all pairs of modified Rankin Scores (mRS) categories
Setting
- 41 Hospitals in Europe (Netherlands, UK, France)
- Feb 2009 – Oct 2015
Population
- Inclusion criteria:
- Adult patients
- Non-traumatic supratentorial intracerebral haemorrrhage confirmed with brain imaging
- GCS 8-15
- Platelet transfusion could be initiated within 6 hours of symptom onset and within 90 minutes of brain imaging
- Had been taking antiplatelet therapy for at least 7 days prior to ICH (COX inhibitor: aspirin carbasalate calcium, ADP receptor inhibitor: clopidogrel, adenosine re-uptake inhibitor: dipyridamole)
- Baseline modified Rankin score of 0 (no symptoms) or 1 (no significant disability)
- Exclusion criteria:
- Blood on brain imaging suggestive of epidural or subdural haematoma
- Underlying aneurysm or AV malformation
- Planned surgical evacuation of ICH within 24 hours of admission
- Intraventricular blood more than sedimentation in the posterior horns of the lateral ventricles
- Previous adverse reaction to platelet transfusions
- Known use of Vitamin K antagonist, unless INR ≤1.3
- History of coagulopathy or platelet <100
- Death appeared imminent
- 190 patients randomised
Comparing baseline characteristics of intervention vs. control groups
- Antiplatelet therapy pre-ICH
- COX inhibitor alone: 73% vs. 84%
- COX inhibitor + dipyridamole: 19% vs. 14%
- Median GCS score: 14 vs. 15
- Age >80: 29% vs. 37%
- ICH volume >30ml: 34% v. 21%
- Intraventicular extension: 13% vs 22%
- Had exclusions to trial entry: 15% vs. 23%
- Intraventricular haemorrhage: 12 patients vs. 20 patients
- Infratentorial location of haematoma: 2 patients vs. 0 patients
- Not taking antiplatelets: 1 patient vs 0 patient
- Thrombocytopenia: 0 patient vs. 1 patient
Intervention
- Platelet transfusion (leucocyte depleted)
- 5 units if on COX inhibitor, 10 units if on ADP receptor inhibitor
- n=97, of whom 4 did not receive platelet transfusion
Control
- Standard care (not defined)
- n=93, of whom 2 received platelet transfusion
Outcome
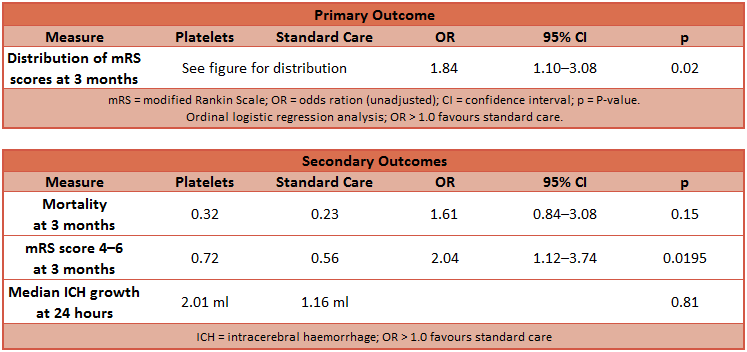
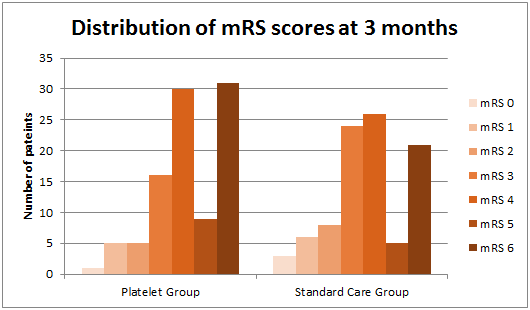
- Primary outcome: difference in functional outcome at 3 months as assessed by mRS
- Odds of a shift towards death or dependence at 3 months significantly higher in the intervention group than in standard care
- Unadjusted OR 1.84, 95% C.I. 1.1-3.08, p=0.02
- Adjusted OR 2.05, 95% C.I. 1.18-3.56, p=0.01
- Odds of a shift towards death or dependence at 3 months significantly higher in the intervention group than in standard care
- Secondary outcomes: Comparing intervention vs. control groups
- Alive at 3 months: 68% vs. 77%, OR 0.62 (0.33-1.19), p=0.15
- mRS score 4-6 at 3 months: 72% vs 56%, OR 2.04 (1.12-3.74), p=0.02, fragility index 2 patients, with number of patients lost to follow up of 0 patients
- mRS score 3-6 at 3 months: 89% vs 82%, OR 1.75 (0.77-3.97), p=0.18
- Median ICH growth at 24 hr (ml) 2.01 vs. 1.16 , p=0.81, however baseline imaging values missing in 7 patients, and repeat imaging values missing in 37 patients
- No significant difference in any serious adverse event
- Overall: 42% vs. 29%, OR 1.79 (95% C.I. 0.98-3.27)
- Thromboembolism: 4% vs. 1% OR 3.96 (95% C.I. 0.43-36.08)
- Complication of ICH: 25% vs. 14% (OR 2.02 (95% C.I. 0.96-4.27)
- Pre-specified sub-group
- Haematoma volume
- <7ml: OR 2.46 (95% C.I 1.02-5.94)
- 7-30ml: OR 1.4 (95% C.I 0.58-3.39)
- >30ml: 0.87 (95% C.I. 0.27-2.76)
- (Odds ratio of >1 favours control group, where as OR <1 favours transfusion)
- Haematoma volume
- Post-hoc analysis
- Primary outcome remained unchanged when the 36 patients who met at least 1 exclusion criteria were removed from analysis: adjusted OR 2.22 (95% C.I. 1.2-4.09), p=0.01
Authors’ Conclusions
- Platelet transfusions cannot be recommended for the treatment of acute ICH in people taking antiplatelets therapy
Strengths
- Randomised controlled trial
- No patients lost to follow up at 3 months
- blinding of assessors of primary outcome
- Randomised control trial with allocation concealment maintained through web based randomisation
Weaknesses
- Primary outcome changed during trial from dicotomised mRS to current one. However, this was changed prior to knowledge of the outcome data
- Differences in the baseline characteristics between the intervention and the control group
- Large numbers of patients randomised who had exclusion criteria
- Non-blinding of clinicians and patients
- Small numbers of patients included
The Bottom Line
- This small randomised controlled trial demonstrated that patients with ICH who are on antiplatelet agents have worse neurological outcomes at 3 months if they are treated with a platelet transfusion compared with standard care alone. The trial has a number of weaknesses but this is the best evidence we have and I do not think we should be using platelet transfusions for these patients outside of a clinical trial.
External Links
- [article] Platelet transfusion versus standard care after acute stroke due to spontaneous cerebral haemorrhage associated with antiplatelet therapy (PATCH): a randomised, open-label, phase 3 trial
- [further reading] St Emlyns journal club
- [further reading] REBEL EM The PATCH Trial
- [further reading] EMLit of Note: Put the Platelets Away in ICH
- [further trial awaited] Platelet Transfusion in Acute Intracerebral Hemorrhage
Metadata
Summary author: @davidslessor
Summary date: 21st June 2016
Peer-review editor: @duncanchambler





Pingback: The PATCH Trial: Hold the Platelets in Spontaneous Intracerebral Hemorrhage? - R.E.B.E.L. EM - Emergency Medicine Blog
Pingback: SGEM#182: Platelet Transfusions for Intracerebral Hemorrhage (PATCH) – Don’t Do It. | The Skeptics Guide to Emergency Medicine