CLASSIC

Restricting volumes of resuscitation fluid in adults with septic shock after initial management: the CLASSIC randomised, parallel-group, multicentre feasibility trial
Clinical Question
- In ICU patients with septic shock who have had initial fluid resuscitation, what are the effects and feasibility of a protocol restricting further resuscitation fluid as opposed to standard care?
Design
- Open label, multicentre, stratified, parallel group clinical trial. Clinicians and patients not blinded
- Computer generated allocation sequence with permuted blocks of 2 or 4
- Web-based centralised randomisation system with stratification by site
- 1:1 randomisation to restrictive protocol or standard care
- Intention to treat analysis
- Several statistical analyses performed:
- Primary outcomes compared using a mix of parametric (general linear model) and non-parametric (van Elteren) methods adjusted for site of randomisation
- Logistic regression, logrank and cox used for secondary outcome measures
- Primary outcomes re-analysed with second model adjusting for certain predefined baseline risk factors (age, weight, norepinephrine dose at randomisation, surgery prior to randomisation, and >5L of fluid given before randomisation)
- Modification of primary outcome occurred one month before the trial ended, with promotion of a secondary outcome (volume of resuscitation fluid during total ICU stay) to a “co-primary” one
- Power calculation:
- 150 patients needed to show 1.7L difference in volume of resuscitation fluid within first 5 days, based on 6S trial data, at a power of 80% and a two sided alpha of 5%
Setting
- Nine general ICUs in Europe (Denmark and Finland)
- September 2014-August 2015
Population
- Inclusion:
- Age >18 years
- Sepsis defined by SCCM/ACCP guidelines 2008 (2 out of 4 SIRS criteria and suspected or confirmed site of infection/positive blood culture)
- Suspected or confirmed circulatory impairment (at least one of SBP<90, lactate >4, HR >140, use of vasopressors)
- At least 30ml/kg IBW fluids (crystalloids, colloid, or blood) given within the last 6 hours
- Shock defined as ongoing infusion of norepinephrine to maintain blood pressure
- Exclusion:
- Use of any form or RRT, or RRT deemed imminent by ICU physician
- Severe hyperkalaemia (>6mmol) within last 6 hours
- Creatinine >350 micromoles/l
- Invasively ventilated with FiO2>0.8 ad PEEP>10
- Life threatening bleeding
- Kidney or liver transplantation during current admission
- Burns >10% BSA
- Previously enrolled in CLASSIC trial
- Patients with treatment limitations (not for mechanical ventilation and RRT)
- Consent unavailable
- 203 patients screened, 153 randomised, 151 in final analysis
Intervention
- Fluid restriction group:
- Isotonic crystalloid fluid boluses of 250-500ml IV allowed during ICU stay for severe hypo perfusion defined by:
- Lactate >4
- MAP<50 despite norepinephrine infusion
- Mottling score >2
- Oliguria of <0.1ml/kg IBW in the last hour
- Isotonic crystalloid fluid boluses of 250-500ml IV allowed during ICU stay for severe hypo perfusion defined by:
Control
- Standard care group:
- Isotonic crystalloid boluses allowed during ICU stay as long as haemodynamic variables improved during dynamic or static measures of fluid responsiveness (whichever the clinician’s choice)
In both groups:
- MAP>65mmHg (or a target decided by clinicians) maintained during ICU stay
- Norepinephrine 1st line vasopressor
- Choice of crystalloid not specified. Colloid seen as protocol violation
- Effect of fluid bolus monitored 30 minutes after intervention
- Concomitant treatments for sepsis (other vasopressors, inotropes, glucocorticoids, blood products, RRT, interventions for AF) provided based on SSC guidelines 2012
- Overt fluid losses (bleeding, diarrhoea, ascites, pleural effusion) allowed to be substituted
- Electrolytes/water supplements recommended enterally
- IV isotonic glucose allowed if total fluid input <1500ml and enteral supplementation not possible
- Protocol temporarily suspended during life-threatening bleeding
Outcome
- Co-Primary outcomes: amount of resuscitation fluid used in first 5 days and over length of ICU stay post randomisation was significantly less in the fluid restricted group
- First 5 days:
- Fluid Restricted Group:
- median 500 ml [IQR 0–2,500 ml]
- site-weighted mean was 1,687 ml
- Standard Care Group:
- median 2,000 ml [IQR 1,000–4,100 ml]
- site-weighted mean 2,928 ml
- Absolute difference in mean: -1,241 ml (95% CI -2,043 to -439 ml)
- P value (non-parametric test) < 0.001
- Fluid Restricted Group:
- During entire ICU stay:
- Fluid Restricted Group:
- median 500 ml [IQR 0–3,250 ml]
- site-weighted mean was 1,992 ml
- Standard Care Group:
- median 2,000 ml [IQR 1,000–4,750 ml]
- site-weighted mean 3,399 ml
- Absolute difference in mean: -1,407 ml (95% CI -2,358 to -456 ml)
- P value (non-parametric test) < 0.001
- Fluid Restricted Group:
- First 5 days:
- Secondary outcomes: No significant difference in total fluid inputs and cumulative balances during first 5 days or overall ICU stay
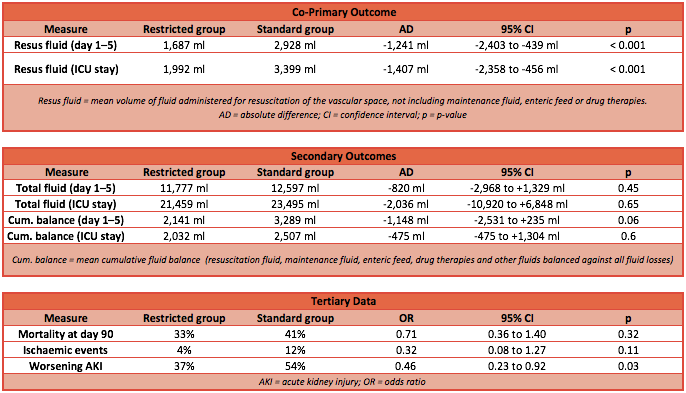
- Adverse incidents: No significant differences in adverse reactions to crystalloids, norepinephrine, or ischaemic events
- Exploratory outcomes:
- Death at day 90, ischaemic events, days alive without mechanical ventilation or RRT, maximum changes in plasma creatinine – no significant difference
- Worsening of acute Kidney injury (defined by KDIGO score) significantly lower in fluid restriction group
Authors’ Conclusions
- A protocol aimed at restricting resuscitation fluid is feasible and resulted in reduced volumes of resuscitation fluid compared to a protocol aimed at standard care of ICU patients who had undergone initial resuscitation.
Strengths
- An important clinical question – especially after the FEAST trial which suggested harm from large volume fluid resuscitation
- Multisite, multi-country trial
- Care broadly standardised between groups
- Clear separation in practice achieved between groups, despite the lack of blinding
- Intention to treat analysis – Only 2 patients excluded
Weaknesses
- Lack of blinding – leading to significant clinician leeway over MAP targets, co-interventions, and fluid responsiveness targets. While this reflects “real world” practice, it does reduce the internal and external validity of the trial data.
- Adding a co-primary outcome measure just before the trial ended. While this did not affect the actual recorded primary outcome, the trial was not designed to examine this variable.
- Despite trial conditions, a significant number of protocol violations were observed – 34 patients (45%) in the restrictive group, and 23 patients (30%) in the control group. This considerably reduces the impact of the intervention. Most notably:
- 27 patients (36%) in the intervention groups received fluid boluses outside indication
- 16 restrictive patients (21%) and 18 control patients (24%) received colloids.
- There was no significant difference in total fluid given to both groups of patients either during the first 5 days or overall during their ICU stay. The 1L deficit in resuscitation fluid seems to have been corrected for elsewhere (NG feeding and fluids with medication). The restrictive group may not have been truly restricted after all.
The Bottom Line
- This trial demonstrated the feasibility of a fluid restrictive strategy post initial resuscitation of patients with septic shock.
- However, a truly restrictive strategy seems difficult to implement without protocol violations, and total fluid volumes were actually no different between the groups. In this trial this makes safety of this approach difficult to truly gauge.
- A strategy of limiting any post-resuscitation fluid to patients who are either fluid responsive or tolerant, using dynamic indices of fluid responsiveness, seems to be supported by this trial, and by other available data from the FEAST and FACTT trials. This will remain my current strategy.
External Links
- [article] Restricting volumes of resuscitation fluids in adult with septic shock after initial management: the CLASSIC randomised, parallel-group multi centre feasibility trial
- [further reading] Acheampong A, Vincent JL. A positive fluid balance is an independent prognostic factor in patients with sepsis.
- [further reading] Maitland K et al. Mortality after fluid bolus in African Children with Severe infection.
- [further reading] Hoste EA et al. Four phases of intravenous fluid therapy: a conceptual model.
- [further reading] Effect of an Early Resuscitation Protocol on In-hospital Mortality Among Adults With Sepsis and Hypotension A Randomized Clinical Trial
Metadata
Summary author: Segun Olusanya
Summary date: 6 October 2016
Peer-review editor: Duncan Chambler




Pingback: Clinical Trials in Intensive Care (Tuesday) | LIVES 2016
Thanks for this excellent summary. Ever since the publication of the Murphy study in Chest in 2009 (https://www.ncbi.nlm.nih.gov/pubmed/19318675) there is increasing awareness on the deleterious effects of fluid overload. Albeit retrospective this landmark study was hypothesis generating and showed that the patients who received early adequate fluid management (30 ml/kg/6-8 hours) followed by late conservative fluid therapy (defined as 2 consecutive negative daily fluid balances during the first week) carried the best prognosis. This led to looking at fluids beyond their mere role for resusciattion but as drugs, with the 4 D’s in analogy to antibiotics (https://journals.viamedica.pl/anaesthesiology_intensivetherapy/article/viewFile/AIT.a2015.0070/30252): not only the type of fluid, but also the dose, the speed of administration (eg fluid bolus vs maintenance), the duration of fluid therapy and de-escalation. This has been referred to as the 4 (or even 5) phases of fluid therapy with the last phase called DE-resuscitation (https://www.ncbi.nlm.nih.gov/pubmed/25432556). See also related blog on DE-resuscitation on Life in the Fast Lane (http://lifeinthefastlane.com/ccc/de-resuscitation-and-positive-fluid-balance/).
Manu,
Thanks for your comment and discussion. This area is evolving and it is become clear that fluid is not a benign therapy. I look forward to the IFAD conference to discuss this and more! (COI: Manu’s invited me to the conference to assist with the social media broadcast).