CHECK-UP Checklist

A Multicenter Randomized Trial of a Checklist for Endotracheal Intubation of Critically Ill Adults
Jane. Chest 2017; Published first online. doi:10.1016/j.chest.2017.08.1163
Clinical Question
- In critically ill patients undergoing intubation, does the use of a pre-intubation checklist compared to no checklist prevent oxygen desaturation or systolic hypotension?
Background
- Complications occur in up to one-third of critically ill patients undergoing airway intubation, with hypoxaemia and hypotension being the most common event
- Operator inexperience and inadequate preparation are associated with increased incidence of complications
- A checklist is a cheap intervention that can improve non-technical “human” factors during times of stress and high-intensity mental activity
Design
- 2 x 2 factorial design
- Other side of the study assessed the effect of the ramped position vs the sniffing position for intubation of the critically ill adults: CHECK-UP-position
- Randomised, multicentre pragmatic trial
- Patients randomised in a 1:1 ratio using a computer and permuted blocks
- Data collected by an independent observer, with quality/accuracy assurance carried out on 11% of the cases
- 248 patients required to power the study at 80% to detect a difference between the two groups in lowest recorded saturation of 5%
- 5% chosen based on previous similar studies
- Initial power calculations required only 170 patients
- After assessment of the standard deviations (SD) of the primary outcome for the whole study population at 6 months, the SD was larger than anticipated so a new power calculation was performed
- Group assignments remained concealed
- With respect to the lowest systolic blood pressure (SBP), 260 patients gave a 76.4% power to detect a 10mmHG difference in SBP between groups
Setting
- Five tertiary ICUs in the United States
- Three of which were part of the factorial design with CHECK-UP-position, whilst the other two only randomised for CHECK-UP-checklist
- July 2015 to July 2016
Population
- Inclusion: Patients over the age of 18 undergoing endotracheal intubation by critical care fellows or pulmonary fellows or anaesthetic residents in the ICU
- Exclusion:
- If awake intubation planned
- If intubation was so urgent that the clinician felt the randomisation envelope could not be obtained in time
- Or if the clinician felt a specific checklist was required based on clinical need
- 318 patients eligible, 51 excluded, 267 randomised, 262 analysed
- 5 were excluded after randomisation
Intervention
- Pre-intubation checklist
- A printed checklist was read aloud by a team member with a verbal acknowledgement of each item by the person performing the intubation
- The checklist contained 10 items focusing on the set up and non-technical skills
- It did not dictate technique, medications or method for pre-oxygenation
- The checklist had to be performed prior to the administration of the procedural medications
- Operators could abort the checklist at any point if they thought the clinical situation required so
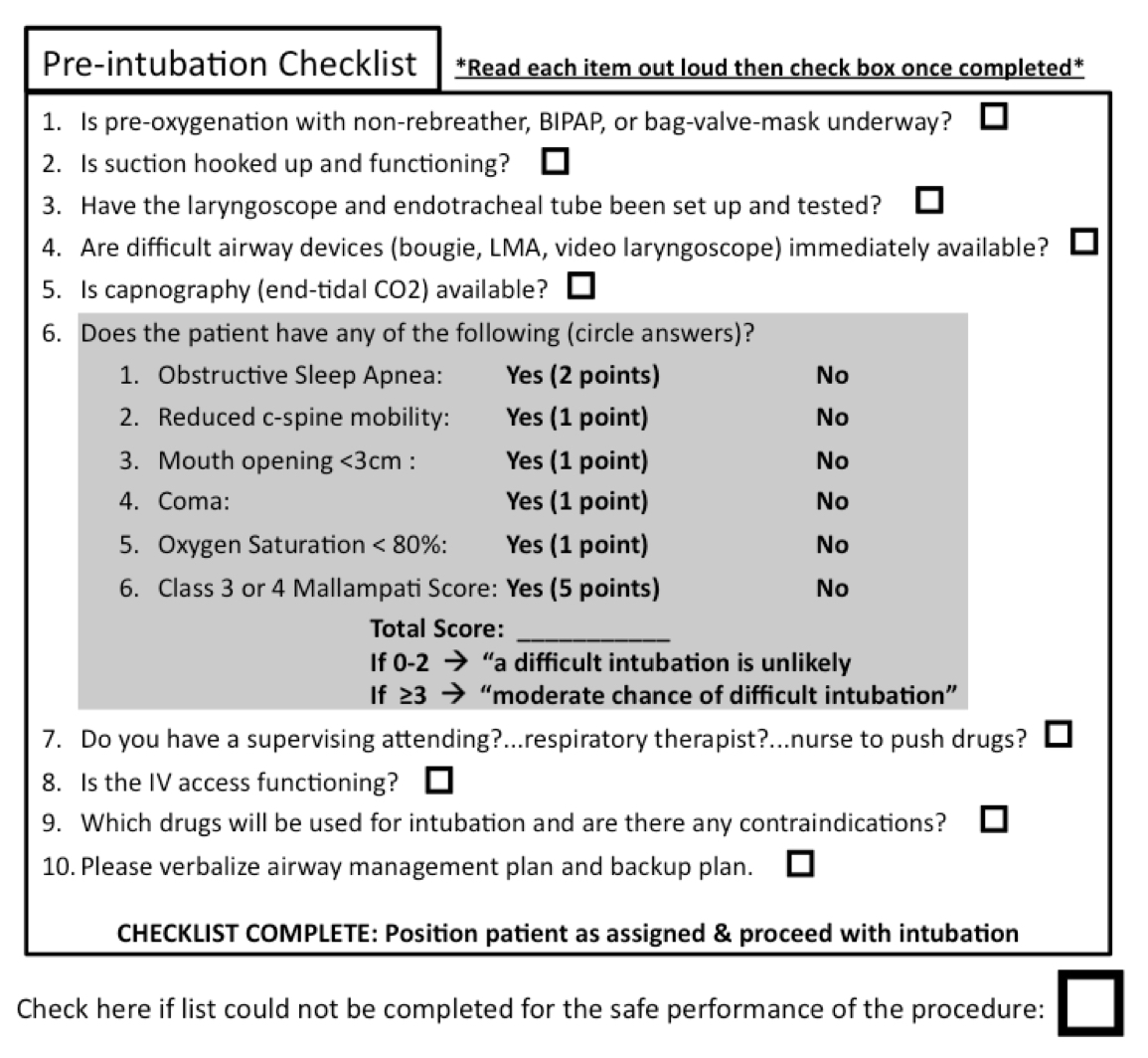
Checklist used for CHECK-UP-checklist trial. Copied from the supplementary datasheet at http://journal.chestnet.org/cms/attachment/2113566199/2084333848/mmc1.pdf
Control
- Usual care
- No structured, verbalised checklist was used
Management common to both groups
- All aspects of the intubation procedure were at the discretion of the clinical team
- Measurement of primary outcomes took place from the moment the procedural medications were administered until two minutes after successful intubation
Outcome
- Primary outcome:
- There was no significant difference in the co-primary outcomes of the lowest median saturation recorded and the lowest SBP
- Lowest median saturation
- Checklist 92% [IQR 79-98] vs Usual Care 93% [IQR 84-100] (P = 0.34)
- Lowest SBP
- Checklist 112 mmHg [IQR 94-133] vs Usual Care 108 mmHg [IQR 90-132] (P = 0.61)
- Lowest median saturation
- This still held true after adjusting for cofounders including BMI, APACHE II score and operator experience
- There was no significant difference in the co-primary outcomes of the lowest median saturation recorded and the lowest SBP
- Secondary outcome:
- Use of the checklist did not decrease number of attempts, shorten time to intubation or improve the Cormack-Lehane view
- No statistically significant difference in life-threatening complications such as cardiac arrest or severe hypotension
- Tertiary data, subgroup or post-hoc analyses:
- No statistically significant difference in tertiary outcomes of ventilator free days, ICU days or in-hospital mortality
Authors’ Conclusions
- The use of a verbally performed pre-intubation checklist was not associated with a reduction in complications or an improvement in clinical outcomes
Strengths
- Prospective, multicentre, randomised study with large numbers
- Sensibly focussed on trainees only as they are more likely to benefit from an intubation checklist and will often be the first line operator
- Although they did not include truly ‘novice’ trainees, as the least experienced trainee had performed 32 intubations prior to the study
- Pragmatic and transparent approach to the design of the checklist
- Independent observer collected data to limit bias from unblinded methodology
- Quality assurance took place to check accuracy of data collection
Weaknesses
- Factorialised design
- Although there was no interaction between the patient position and the use of a checklist (p=0.94), they both assessed the same primary outcome
- Only some patients were part of factorial intervention
- This complex methodology may have reduced the power to detect a true benefit from either one intervention
- 19% of intubations assigned to the checklist arm did not complete the full checklist
- Only 2 were due to increasing urgency of the intubation
- No reason documented for the other 22 cases
- The study was impossible to blind
- Group allocation may have influenced the unblinded intubating clinician behaviour
- This was analysed post-hoc and showed no difference in the primary outcomes
- The checklist items were largely performed in the intubations carried out without the checklist, suggesting there was penetration of the intervention into the usual care group
- This would tend to reduce any difference and bias towards the null hypothesis
The Bottom Line
- This study suggests that the use of a pre-intubation checklist does not reduce any peri-procedural complications and may even delay the intubation
- The use of checklists should not be discouraged based on this trial alone, as there may be other benefits that have not been measured in this trial
External Links
- [article] A multicenter randomized trial of a checklist for endotracheal intubation of critically ill adults
- [further reading] NAP4 Report regarding complications of airway management by Royal College of Anaesthetists (UK)
- [further reading] RSI Checklists and Action Plans from LITFL
Metadata
Summary author: Alex Smith
Summary date: 02 November 2017
Peer-review editor: Duncan Chambler




In my opinion , using verbally performed pre-intubation checklist any way will increase the safety of the procedure especially in area where there is lack of clear intubation protocol. It is an excellent study regarding of the outcome did not showed any difference between both groups.