VANISH Trial

Effect of Early Vasopressin vs Norepinephrine on Kidney Failure in Patients With Septic Shock
The VANISH Randomized Clinical Trial
Gordon. JAMA. 2016;316(5):509-518. doi:10.1001/jama.2016.10485
Clinical Question
- Does early vasopressin use reduce the risk of kidney failure in patients with septic shock compared with norepinephrine?
Design
- Factorial (2×2) multicenter, double blind, randomised controlled trial
- Patients were assigned to 1 of 4 treatment groups on a 1:1:1:1 basis with variable block size randomisation (4 and 8) using computer-generated numbers, stratified by center
- Intention to treat analysis
- A sample size of 400 provided 80% power to detect a 20% to 25% relative reduction of risk of developing kidney failure if treated with vasopressin compared with norepinephrine, assuming an overall incidence of acute kidney failure of 30-50% and a significance level of 0.05
Setting
- 18 adult general ICU’s
- February 2013 – May 2015
Population
- Inclusion: Adult patients (≥16 years) who had sepsis (2 of 4 systemic inflammatory response criteria due to known or suspected infection) and who required vasopressors despite adequate intravenous fluid resuscitation. Enrollment into the trial within 6 hours
- Exclusion: patients who had received a previous continuous infusion of vasopressors during this ICU admission; requirement for systemic steroid treatment (e.g adrenal insufficiency or regular systemic steroid therapy within the last 3 months); end-stage kidney failure; known mesenteric ischaemia; Raynaud phenomenon; systemic sclerosis; other vasospastic disease; known pregnancy
- 421 patients were randomised of which 409 patients were included in the study
Intervention
- Open labelled vasopressor was permitted for up to 6 hours before enrolment to this study. Once study drug one was commenced, the open labelled vasopressor was weaned off as quickly as possible
Study drug 1
- Vasopressin (titrated up to 0.06 U/min) or Norepinephrine (titrated up to 12 μg/min)
- administered via a central venous catheter
- titrated to maintain the target mean arterial pressure 65 to 75 mm Hg, but this could be altered by the treating physician
Study drug 2
- Hydrocortisone (50mg 6 hourly and then weaned) or Placebo
- study drug 2 was administered once the maximum infusion rate of study drug 1 was reached
- administered as an intravenous bolus every 6 hours for 5 days, every 12 hours for 3 days, and then once daily for 3 days
- study drug 2 could be weaned more quickly if the shock had already resolved
In all groups
- If the patient was still hypotensive after the first dose of study drug 2 then additional open-label catecholamine vasopressors could be administered
- Open-label catecholamine vasopressors were reduced first and only once the patient was weaned off open-label vasopressors was study drug 1 then reduced
Outcome
- Primary outcome: the number of days alive and free of kidney failure (defined by AKIN group stage 3) separated into two outcome measures:
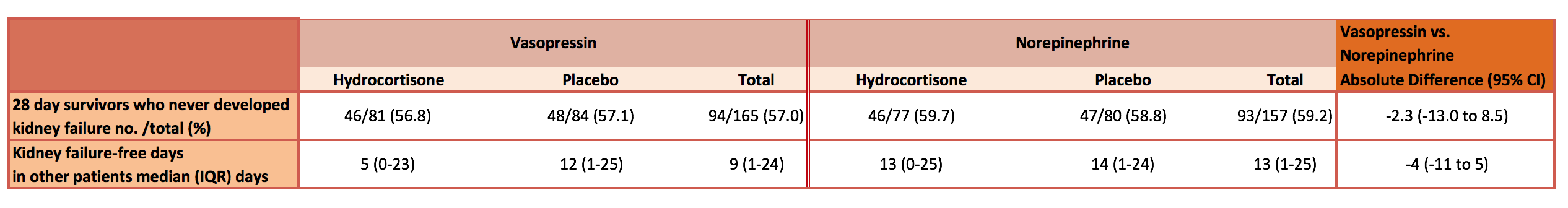
- 28 day survivors who never developed kidney failure: no difference between groups
- vasopressin + hydrocortisone: 56.8%
- vasopressin + placebo: 57.1%
- Norepinephrine + hydrocortisone: 59.7%
- Norepinephrine + placebo: 59.2%
- Vasopressin vs. Norepinephrine absolute difference: -2.3 [95% CI -13.0 to 8.5]
- median number of days alive and free of kidney failure for those patients that did not survive and/or who experienced kidney failure
- vasopressin + hydrocortisone: 5 days (IQR 0-23)
- vasopressin + placebo: 12 days (IQR 1-25)
- Norepinephrine + hydrocortisone: 13 days (IQR 0-25)
- Norepinephrine + placebo: 14 days (IQR 1-24)
- Vasopressin vs. Norepinephrine absolute Difference: −4 days [95% CI −11 to 5]
- 28 day survivors who never developed kidney failure: no difference between groups
- Secondary outcomes: Fewer patients required renal replacement therapy in the vasopressin group compared with the norepinephrine group. These patients were mostly the non-survivors
- Other secondary outcomes: no significant difference between groups for:
- 28 day, ICU or hospital mortality rates
- Kidney failure rate
- Use of inotropes and shock reversal
- Mean SOFA scores
- Duration of mechanical ventilation
- ICU and hospital length of stay
- Serious adverse events (including digital or mesenteric ischaemia, life-threatening arrhythmia and acute coronary syndrome)
- 10.7% in the vasopressin group vs 8.3% in the norepinephrine group; difference, 2.5% [95% CI, −3.3% to 8.2%]
Authors’ Conclusions
- Among adults with septic shock,the early use of vasopressin compared with norepinephrine did not improve the number of kidney failure–free days
Strengths
- An important clinical question comparing vasoactive drugs and the interaction of corticosteroids in patients with septic shock
- Drug ampoules were masked by overlabeling on the body and neck of normal drug ampoules. Matching placebo ampoules were used
- All clinical staff and researchers were blinded
- The baseline characteristics of the groups were well matched for APACHE II score, co-morbidities (including risk of renal injury such as pre-exisiting chronic kidney disease and diabetes), median fluid volume received in the first 4 hours and infection source (primarily lung)
Weaknesses
- Timing of initiation of renal replacement therapy and levels of haemodynamic monitoring were not controlled, other than specifying that sites should follow the international guidelines
- Short time outcomes (28 day and hospital mortality) were assessed and therefore any long-term differences between treatment groups cannot be assessed
- No health economic analysis – the lower rate of renal replacement therapy in the vasopressin-treated patients could be important
- 72% of patients received study drug 2. Only 35% of patients received steroid treatment. The power to assess an interaction between steroids and vasopressors, particularly vasopressin is therefore limited
The Bottom Line
- Early vasopressin maintains blood pressure and reduces the requirement for norepinephrine and renal replacement therapy. However, vasopressin does not reduce the number of renal replacement free days or mortality rate, and there was no clinical interaction with corticosteroids
External Links
- [abstract] Effect of Early Vasopressin vs Norepinephrine on Kidney Failure in Patients With Septic Shock: The VANISH Randomized Clinical Trial
- [trial protocol] Protocol for a randomised controlled trial of VAsopressin versus Noradrenaline as Initial therapy in Septic sHock (VANISH)
- [Podcast] VANISH. Presented by Tony Gordon at State of the Art 2015
- [further reading] VASST: Vasopressin versus Norepinephrine Infusion in Patients with Septic Shock
Metadata
Summary author: Steve Mathieu
Summary date: 4th August 2016
Peer-review editor: Duncan Chambler




Pingback: VASST – The Bottom Line
Pingback: Pulmcrit - Renoresuscitation, vasopressin, vepinephrine, and VANISH
Pingback: Squeezing the Kidneys in Septic Shock - Intensive Care Network
Pingback: Steroids in Sepsis – The Bottom Line