DREAMS

Dexamethasone versus standard treatment for postoperative nausea and vomiting in gastrointestinal surgery
DREAMS Trial Collaborative. BMJ 2017; 357:j1455. doi:10.1136/bmj.j1455
Clinical Question
- In patients undergoing bowel surgery, does a single dose of dexamethasone compared against standard care reduce nausea and vomiting in the early post-operative period?
Background
- Nausea and vomiting is common after bowel surgery due to a multitude of factors
- Dexamethasone has been shown to be an effective anti-emetic in small studies or in studies where few patients underwent bowel surgery
- A key component of the Enhanced Recovery After Surgery (ERAS) programme is to establish oral diet and normal bowel function early, which can be impaired due to nausea and vomiting and consequently delays patient recovery and increases hospital resource use
Design
- Randomised, controlled clinical trial
- Computerised, central randomisation method with minimisation procedure to reduce the risk of chance imbalances (using variables of gender, smoking status, type of surgery, analgesia strategy, ASA grade and participation in ERAS pathway)
- Concealment of allocation until after induction of anaesthesia and administration of any standard anti-emetic
- Blinding of all staff except anaesthetist, who was instructed to keep allocation to themselves and were not involved in post-operative care of the patient
- Intention to treat analysis
- 6 (0.4%) lost to follow-up
- Initially powered at 80% but higher than expected recruitment rates allowed an increase in power to 90%
- Target sample size 1320
- 90% power (I.e. 10% chance of false negative conclusion)
- Two tailed significance testing at 0.05 level (I.e. 5% chance of false positive conclusion)
- 10% loss to follow-up expected
- Based on baseline post-operative vomiting rate of 37% and an expected absolute difference of 9%
Setting
- 45 hospitals across the UK
- July 2011 to January 2014
Population
- Inclusion: Adults over 18 years undergoing elective open or laparoscopic surgery for malignant or benign bowel pathology
- Exclusion: Bowel obstruction, diabetes, glaucoma, gastric ulceration (endoscopically diagnosed), known adverse reaction to dexamethasone, systemic steroids (not inhaled or topical steroids) within last three months
- 2,901 screened -> 1,350 recruited and randomised -> 1,344 analysed
- Patient demographics, anaesthetic and surgical variables were similar between the two groups (Dexamethasone vs Standard Care)
- Mean age: 63 years vs 63 years
- Gender: 42% female vs 42% female
- Smoker: 15% vs 15%
- ASA 1 or 2: 83% vs 83%
- Laparoscopic approach: 64% vs 63%
- ERAS: 91% vs 91%
- Mean duration of anaesthesia: 226 min vs 226 min
- Anti-emetics
- Ondansetron: 78% vs 69%
- Cyclizine: 5% vs 5%
- Other single drug: 3% vs 4%
- Multiple drugs: 8% vs 20% (contrary to protocol)
Intervention
- Dexamethasone
- 8 mg Dexamethasone intravenously administered after induction
Control
- Standard Care
- No Dexamethasone administered
Management common to both groups
- All patients underwent general anaesthesia
- A single dose of a routine anti-emetic was administered at the discretion of the anaesthetist (prior to revealing the patient’s allocation)
- No further anti-emetic was administered during the procedure
- Post-operative anti-emetics were administered at the request of the patient
- Treating anaesthetists were not involved in post-operative care unless required for emergencies
- Dexamethasone was not allowed for the first 24 hours after surgery
Outcome
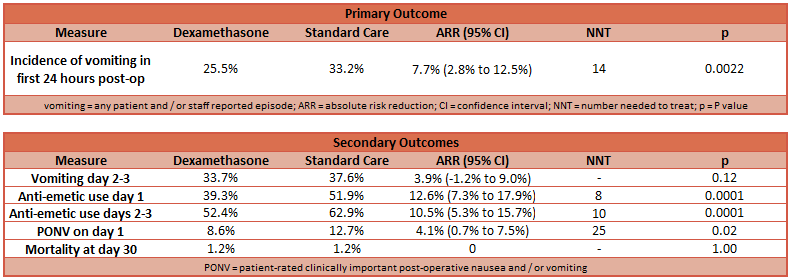
- Primary outcome: any vomiting within 24 hours after surgery
- Dexamethasone: 25.5%
- Standard Care: 33.2%
- Absolute Risk Reduction (ARR): 7.7% (95% CI 2.82% to 12.53%; P = 0.0022)
- Number needed to treat (NNT): 14
- Fragility Index (FI): 18
- Secondary outcome:
- Incidence of vomiting on days 2–3 was not different between groups
- Anti-emetic administration was less in the Dexamethasone group on days 1–3
- Patient-rated clinically significant PONV was less in the Dexamethasone group
- No difference in mortality was seen
Authors’ Conclusions
- The administration of 8mg Dexamethasone in addition to standard anti-emetic care reduces the incidence of nausea and vomiting without increasing adverse events
Strengths
- Multi-centre, randomised, controlled trial
- Ideal randomisation process with event distribution of known variables
- Patient and assessing staff appropriately blinded
- Appropriate statistical tests for variable types
- Excellent recruitment rate, which allowed increased statistical power
- Clinically meaningful and patient-centered outcomes
Weaknesses
- Treating anaesthetist was not blinded to allocation
- The authors argue this allowed an easy to implement, pragmatic study that did not require matching dexamethasone and placebo ampoules to be distributed
- The significant difference in anti-emetic administration between the groups, which was off-protocol, suggests that anaesthetists managed the patients differently after the allocation had been revealed to them
- This may have introduced a bias that would have tended to reduce the measured effect (possibly leading to a false negative conclusion)
- Therefore, dexamethasone may actually have a bigger clinical effect than that identified in this trial
- By excluding diabetic patients, we cannot extrapolate these findings to patients with diabetes, as the harm from peri-operative hyperglycaemia may exceed the benefit from reduced PONV
- The study population underwent planned surgery by mostly laparoscopic approaches, although it may be reasonable to extrapolate that dexamethasone may benefit in emergency cases and open surgical approaches
The Bottom Line
- Dexamethasone 8mg at induction reduces nausea and vomiting after planned bowel surgery and I will be giving this routinely to my patients, so long as they don’t have diabetes
- PONV risk can be stratified and I choose a multimodal approach individualised to each patient’s risk, which includes dexamethasone
- Peri-operative care can influence cancer recurrence and long-term outcomes from dexamethasone administration need to be researched
External Links
- [article] Dexamethasone versus standard treatment for postoperative nausea and vomiting in gastrointestinal surgery (DREAMS Trial)
- [further reading] BJA Education: Nausea and vomiting after surgery by Pierre and Whelan
- [further reading] A Factorial Trial of Six Interventions for the Prevention of Postoperative Nausea and Vomiting: The IMPACT trial by Apfel et al
Metadata
Summary author: Duncan Chambler
Summary date: 19 October 2017
Peer-review editor: Adrian Wong



The big question for me is whether the short-lived benefit in terms of PONV is justified given the long term uncertain impact on cancer recurrence. What would the patient want? Can another antiemetic have the same effect without the risk. The trial makes me less likely to use dex in cancer surgery – the the answer is still up in the air. I believe all cancer patients in this study should be followed up to determine whether dex impacted recurrence.
We here participated in the trial towards the very end. I am deeply skeptical about the design, and the running of the trial.
Example: Contacting the CTU, after about 80% of their patients were recruited, they were not able to define in detail their major outcome markers, i.e. what constitutes vomiting, how to count or delineate possible repeated episodes etc. Their comment: we leave the definition at the discretion of the local clinician. We are only talking about their primary outcome marker here…..
So, what about wretching, but not actually vomiting, or having severe nausea for hours, but not vomiting? No answer from the CTU how to log those…Or having symptoms that come and go: is this one episode, or several. Again, not able to give any guidance or standard!
Amendments to the protocol were still being issued weeks after the trial had stopped recruiting (!), and recruitment stopped almost 4 years ago, so what took them so long to publish this?