CHECK-UP Position
 A Multicenter, Randomized Trial of Ramped Position vs Sniffing Position During Endotracheal Intubation of Critically Ill Adults
A Multicenter, Randomized Trial of Ramped Position vs Sniffing Position During Endotracheal Intubation of Critically Ill Adults
Semler. Chest 2017; 152(4):712-722. doi: 10.1016/j.chest.2017.03.061
Clinical Question
- In critically ill patients undergoing emergency intubation, does the ramped position compared to sniffing position reduce the incidence of oxygen desaturation?
Background
- Hypoxaemia occurs in nearly 50% of Critical Care intubations
- Patient position may improve variables such as functional residual capacity and laryngeal anatomy
- Observational data support the ramped position (torso and head elevated) compared to the sniffing position (patient supine, neck flexed and head extended)
Design
- 2 x 2 factorial design
- Other side of the study assessed the use of an intubation checklist vs standard care in the critically ill adults: CHECK-UP Checklist
- Randomised, multicentre pragmatic trial
- Patients randomised in a 1:1 ratio using a computer and permuted blocks
- Data collected by an independent observer, with quality/accuracy assurance carried out on 10% of the cases
- 248 patients required to power the study at 80% to detect a difference between the two groups in primary outcome of 5%
- 5% chosen based on previous similar studies
- Initial power calculations required only 170 patients
- After assessment of the standard deviations (SD) of the primary outcome for the whole study population at 6 months, the SD was larger than anticipated so a new power calculation was performed
- Group assignments remained concealed
- Intention to treat analysis
Setting
- Four tertiary ICUs in the United States
- July 2015 to July 2016
Population
- Inclusion: Patients over the age of 18 undergoing endotracheal intubation by critical care or pulmonary fellows in the medical ICU
- Exclusion:
- If intubation was so urgent that the clinician felt the randomisation envelope could not be obtained in time
- If treating clinicians felt that a specific position was clinically indicated
- 309 eleigible, 49 excluded (42 due to urgency, 6 due to specifically indicated intubation position), 260 randomised
- The most common reasons for intubation in both groups were sepsis, altered mental status and pneumonia
Intervention
- Ramped position for intubation
- Electronic bed used to elevate head of the bed to 25 degrees with the lower half of the bed parallel to the floor
- Patient’s head was positioned at the top of the mattress so it hung slightly off the bed with the face parallel to the ceiling
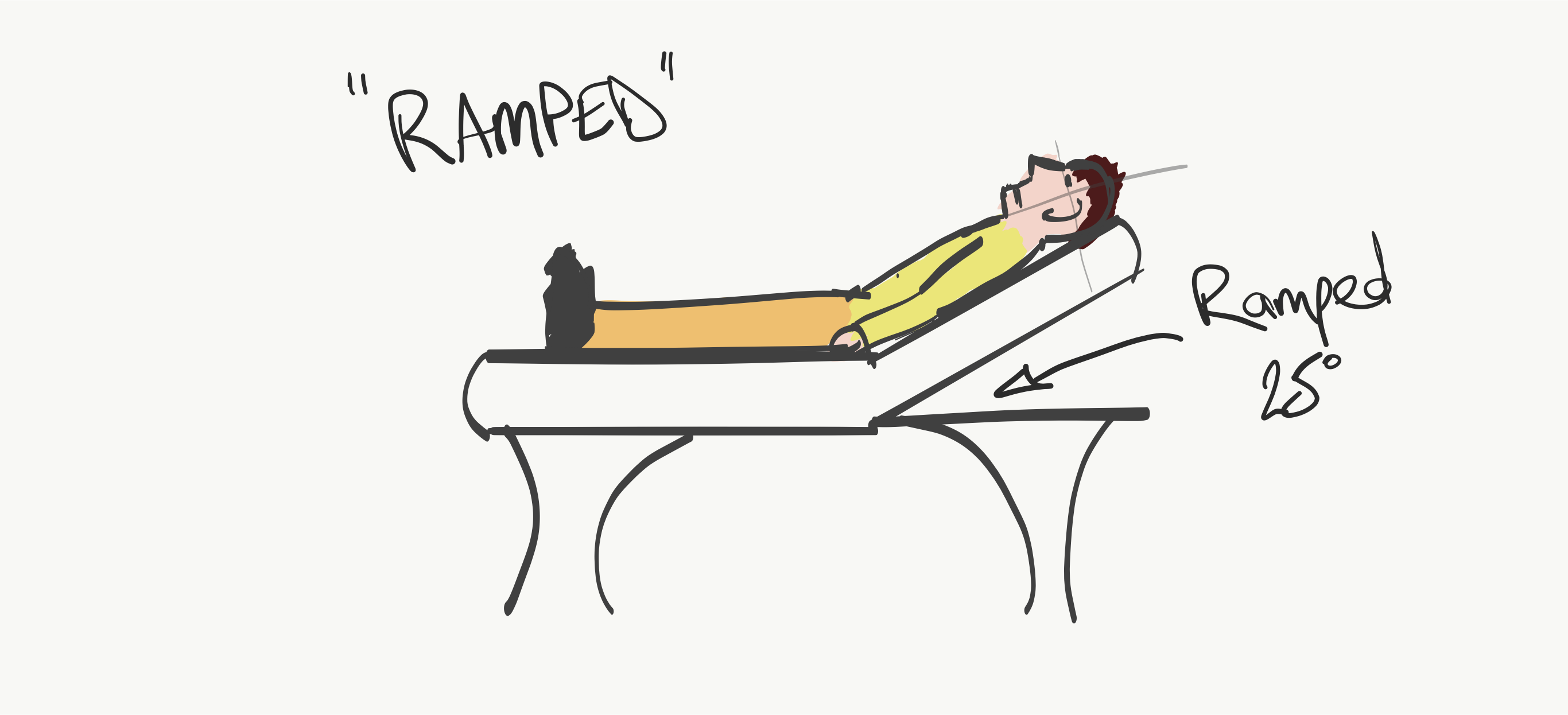
The Ramped Position for Intubation
Control
- Sniffing position for intubation
- Entire bed remained horizontal
- Folded blankets/towels placed beneath the patient’s head with the neck in flexion and the head in extension as if “sniffing the air”.
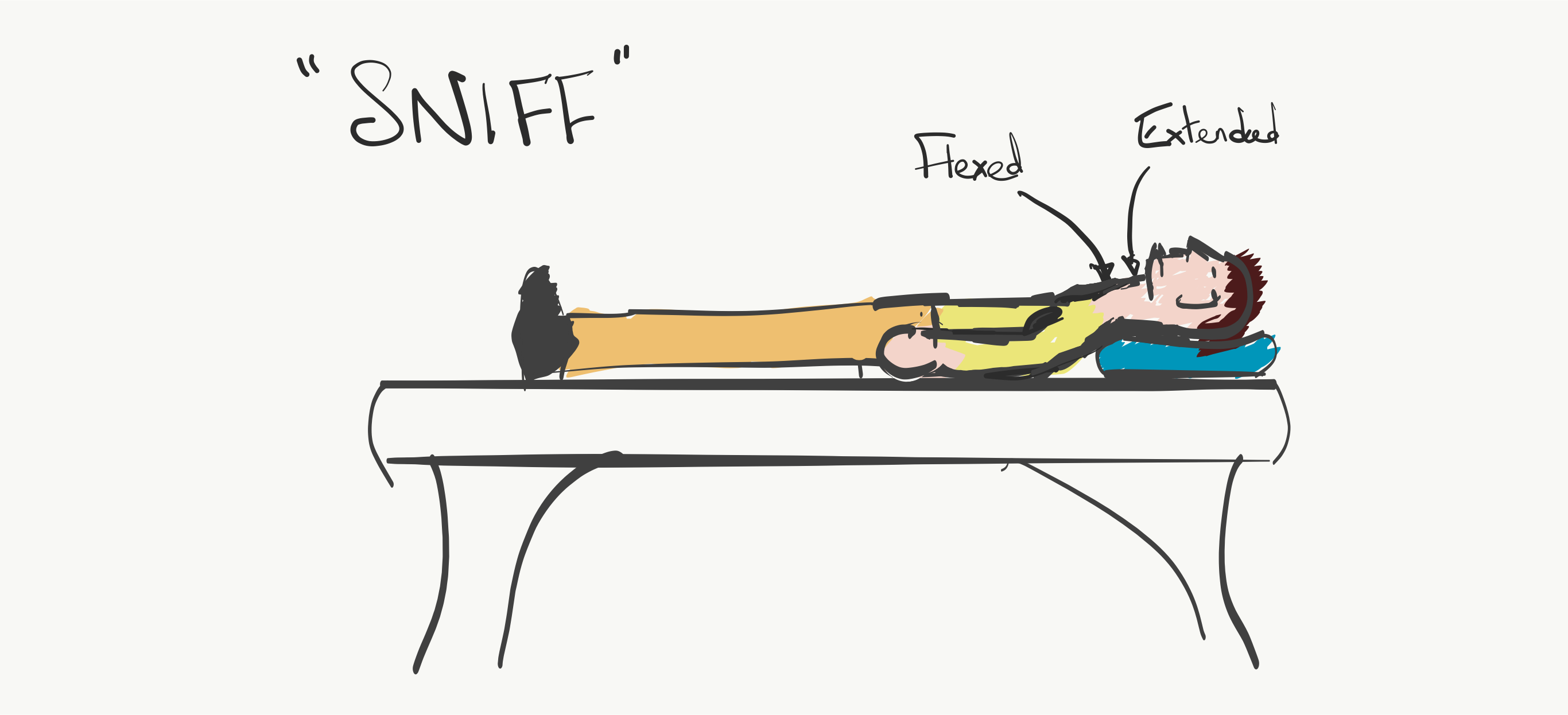
The “Sniffing the Air” Position for Intubation
Management common to both groups
- All aspects of the intubation procedure were at the discretion of the clinical team
- Measures of primary outcomes took place from the moment the procedural medications were administered until two minutes after the successful intubation
Outcome
- Primary outcome: There was no statistically significant difference in the median lowest oxygen saturation between the sniffing and the ramped positions
- Sniffing – 92% [IQR 79-98%]
- Ramped – 93% [IQR 84-99%]
- This still held true after multivariable linear regression analysis to adjust for cofounders including saturation at induction, BMI, operator experience and use of video laryngoscopy
- Secondary outcome:
- The view achieved and difficulty of the intubation was worse in the ramped group
- Cormack-Lehane view Grade III or IV:
- Sniffing 11.6% vs Ramped 25.4% (p=0.01)
- Operator reported “difficult” intubation:
- Sniffing 4.6% vs Ramped 12.3% (p=0.04)
- Cormack-Lehane view Grade III or IV:
- Therefore, the rate of failed intubation attempts was unsurprisingly higher in the ramped group
- First attempt success:
- Sniffing 85.4% vs Ramped 76.2% (p=0.02)
- More than 3 attempts at laryngoscopy:
- Sniffing 2.3% vs Ramped 7.7% (p=0.02)
- First attempt success:
- No difference between other oxygenation or haemodynamic secondary outcomes
- Oxygenation outcomes
- Incidence of hypoxia or severe hypoxia, desaturation and absolute change from baseline saturation
- Haemodynamic outcomes
- Lowest systolic BP, systolic BP <65, use of a vasopressor and cardiac arrest within 10mins of intubation
- Oxygenation outcomes
- The view achieved and difficulty of the intubation was worse in the ramped group
- Tertiary data, subgroup or post-hoc analyses
- No statistically significant difference in tertiary outcomes of ventilator free days, ICU days or in-hospital mortality
- In post-hoc analysis, the operator’s previous intubating experience did not alter the primary outcome
- Similarly, the operator’s prior experience in the ramped position did not alter the primary outcome
- Although this data was only available for 73.8% of the intubations carried out
Authors’ Conclusions
- The ramped position was not associated with an increase in the lowest arterial saturation during intubation of critically ill patients in the ICU, but it may increase the difficulty of the intubation and the likelihood of repeated attempts
Strengths
- Relevant question for daily ICU practice, especially as data from the anaesthetic room does not always translate well to the ICU
- Prospective, multicentre study with larger numbers than similar trials in the anaesthetic room
- First study of its kind in the ICU
- Baseline characteristics well balanced between the two groups, importantly including pre-oxygenation method, APACHE II score, BMI and difficult airway characteristics
- Minimal deviation from protocol (3 total)
- Quality assurance took place to improve accuracy of data collection.
Weaknesses
- Factorialised design
- Although they claim that there was no interaction between the position and the use of a checklist (p=0.94), they both assessed the same primary outcome
- Would have been better to do these two studies separately
- Incomplete data for the clinician’s past experience with the ramped position as it was only available for 73.8% of cases
- Only included fellow/trainee clinicians
- Would have been better to also include those performed by the more senior clinicians
- Cases where the senior clinician feels that they must have first attempt at intubation are perhaps sicker or more challenging
The Bottom Line
- Among adult ICU patients, the ramped position did not improve the lowest recorded saturations but did increase the difficulty of intubation and the likelihood of repeated attempts
- Despite the ramped position being more technically challenging, this did not translate into any difference in any patient-centred outcomes
- We should therefore still assess each intubation on a case by case basis, factoring in our previous experience and comfort level when choosing patient position for intubating the critically unwell patient
External Links
- [article] A multicenter, randomized trial of ramped position vs sniffing position during endotracheal intubation of critically ill adults
- [further reading] The Case of Anatomic Inaccuracy by CC Nerd (Rory Spiegel)
- [further reading] TBL Summary of other half of factorial trial
Metadata
Summary author: Alex Smith
Summary date: 02 November 2017
Peer-review editor: Duncan Chambler



