FEDORA

Effect of goal-directed haemodynamic therapy on postoperative complications in low-moderate risk surgical patients
Calvo-Vecino. Br J Anaesth 2018; 120:615-616. doi:10.1016/j.bja.2018.01.001
Clinical Question
- In peri-operative patients at low to moderate risk of post-operative complications, does goal-directed haemodynamic therapy using oesophageal doppler monitoring compared to standard care, reduce the incidence of post-operative complications within 180 days?
Background
- The EuSOS observational study demonstrated a Europe-wide post-operative mortality rate of 4%, with wide variation between countries
- Moderate risk procedures account for about 40% of all surgical procedures and up to 30% will develop some degree of post-operative complication such as ileus or infection
- The OPTIMISE trial and associated meta-analysis has suggested that goal-directed haemodynamic therapy (GDHT) reduces the incidence of complications in high-risk procedures but does not reduce mortality
- Different monitoring devices are available and commonly used, including arterial pulse-contour analysis (LiDCO) and aortic blood flow analysis by trans-oesophageal doppler ultrasound (ODM, CardioQ by Deltex)
Design
- Randomised, controlled trial
- Sampling method not described
- Randomisation method used web-based computer system
- Allocation was concealed by opaque sequential envelopes, opened on the day of surgery
- Patients and outcome assessors were blinded to allocation but clinicians that provided intra-operative care were aware of allocation
- Intra-operative care was partly standardised with some elements left to the discretion of the non-blinded clinician for pragmatism
- Sample size calculation based on previous meta-analysis in similar population
- Incidence of complications in intervention group 30% compared to 49% in control group
- 210 patients required to detect a similar 19% difference in incidence
- A significance defined at 0.05
- This would result in 80% Power
- Authors decided to recruit 210 patients for each surgical specialty to allow subgroup analysis with adequate power (840 patients)
- Posthoc orthopaedic subgroup was excluded due to low recruitment rate
- Analysis was conducted on a modified intention to treat (only included those randomised who received study treatment)
- Results expressed as raw and adjusted (after adjustment for known confounders)
- Hypotheses related to secondary outcomes were tested using the Holm-Bonferroni method to avoid false positive conclusions by multiplicity (that is, finding something positive by chance only by repeatedly testing the data in different ways)
- Trial terminated early after the recommendation to stop using 6% hydroxyethyl starch in clinical trials
Setting
- Five hospitals in Spain
- 2011 to 2014
Population
- Inclusion: at least 18 years old; scheduled for major abdominal, urological, gynaecological or orthopaedic surgery under general anaesthetic (both open and laparoscopic surgery included)
- Procedure classified as ‘major’ if one of the following criteria met:
- ≥ 2 hours duration
- Estimated blood loss ≥ 15% blood volume
- ≥ 2 unit red blood cell transfusion requirement
- Procedure classified as ‘major’ if one of the following criteria met:
- Exclusion: emergency surgery; ASA physical status score > 3; contraindication for ODM (including aortic pathology that deems ODM less reliable)
- 496 screened; 450 patients recruited; 428 randomised and received study treatment; 420 analysed
- 22 did not receive allocated therapy
- 8 orthopaedic procedure patients excluded after this subgroup was removed from the study
- Baseline characteristics were similar except for slightly higher ASA scores in the GDHT group (GDHT vs Standard Care)
- Mean age: 66.3 yrs vs 64.2 yrs
- Mean BMI: 27.3 vs 27.2
- ASA Physical Status
- ASA 1: 6.7% vs 16.6%
- ASA 2: 58.4% vs 64.4%
- ASA 3: 34.9% vs 19%
- Surgical procedure
- Gastrointestinal: 150 vs 154
- Urology: 48 vs 38
- Gynaecological: 11 vs 19
- Orthopaedic: excluded posthoc
- Anaesthesia
- Epidural sited: 20.1% vs 21.3%
Intervention
- Goal-directed Haemodynamic Therapy (GDHT) group
- Algorithm-directed care for fluids, vasopressors and inotropes
- Targets were
- Within 10% of patient’s ‘optimised’ stroke volume
- Cardiac index > 2.5 l/min/m2
- Mean arterial pressure > 65 mmHg
- Targets were
- Guided by oesophageal doppler monitoring (ODM) values after training by the manufacturer
- Preload was optimised to achieve maximal stroke volume (SV) using crystalloid ± colloid fluid
- 250 ml bolus of crystalloid fluid was administered
- If a 10% or more increase in SV was observed, the crystalloid fluid bolus was repeated
- If a 10% or more increase was again observed, 250 ml colloid (6% HES) boluses were given thereafter instead of crystalloid
- Fluid boluses were repeated until SV did not increase by 10%
- This was recorded as ‘optimised SV’ and used as the haemodynamic goal until the end of surgery
- Stroke volume was maintained within 10% of ‘optimised SV’
- If SV decreased by 10%, additional 250 ml colloid fluid boluses were given
- Inotropes were started if there was an inadequate response to fluid, to maintain cardiac index (CI) above 2.5 l/min/m2 (which was defined as a minimum safe threshold cardiac output)
- Vasopressors were started if SV was optimised and CI was above minimum safe threshold but mean arterial blood pressure (MAP) was below 65 mmHg
- Patients were reassessed every 5 minutes
- Algorithm-directed care for fluids, vasopressors and inotropes
Control
- Standard Care group
- Continuous infusion of Ringer’s lactate fluid
- 3-5 ml/kg/hr if laparoscopic
- 5-7 ml/kg/hr if open
- Colloid (Voluven 6% hydroxyethyl starch), vasopressors and inotropes at clinician’s discretion
- No cardiac output monitor was used
- Intra-operative goals were defined by the clinician
- Continuous infusion of Ringer’s lactate fluid
Management common to both groups
- Intra-operative anaesthetic care was partly standardised
- Balanced anaesthesia with IV induction and volatile maintenance
- Induction doses were at the clinician’s discretion
- BIS (Bispectral Index) was used and maintenance using Sevoflurane was titrated to BIS 40-60
- Epidural, central venous cannulation and arterial cannulation was at the clinician’s discretion
- Basic monitoring (5-lead ECG, pulse oxymetry, non-invasive BP) was universally applied
- At least one peripheral vein was cannulated
- The following physiological targets were defined:
- SpO2 >=94%
- ‘normothermia’
- Heart rate < 100 bpm
- FiO2 60%
- PaCO2 4.7 to 6.0 kPa
- Positive end-expiratory pressure 4-6 mmHg
- Tidal volume 6-8 ml/kg
- Haemoglobin > 100 g/l (cardiac disease) or 70 g/l (no cardiac disease)
- Blood loss was replaced with ‘colloid’ in an equal volume
Outcome
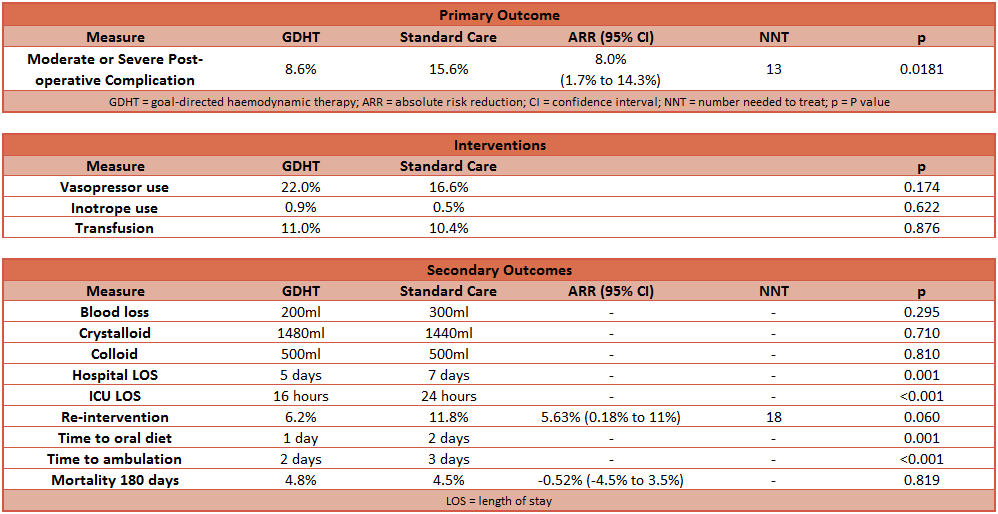
- Primary outcome: the proportion of patients that developed moderate or severe postoperative complications within 180 days of surgery was lower in the GDHT group than in the standard care group
- GDHT group: 8.61%
- Standard Care group: 16.59%
- Absolute Risk Reduction (ARR): 7.98% (95% CI 1.68% to 14.27%; P = 0.0181)
- Number needed to treat (NNT): 13
- Fragility Index (FI): 3
- Secondary outcome: despite no difference in administration of fluids, vasopressors or inotropes, some of the secondary outcomes demonstrate benefit from GDHT
- Vasopressor use: 22.0% vs 16.6%
- Inotrope use: 0.9% vs 0.5%
- Intra-operative red cell transfusion: 11.0% vs 10.4%
- Estimated blood loss was not different between groups
- Crystalloid administration was not different between groups
- Colloid administration was not different between groups
- Length of hospital stay was lower in the GDHT group
- Length of intensive care
stay was lower in the GDHT group - Re-intervention rate was lower but not statistically significant in the GDHT group
- Time to tolerance of oral diet was lower in the GDHT group
- Time to ambulation was lower in the GDHT group
- Mortality at 180 days was not different between groups
Authors’ Conclusions
- Goal-directed Haemodynamic Therapy, using an algorithm based on oesphageal Doppler monitoring, reduces the incidence of moderate or severe post-operative complications in patients at low to moderate risk undergoing major surgery
Strengths
- Appropriate RCT methodology to answer the proposed hypothesis
- The method of randomisation and allocation was good, reducing any selection bias (however, see note below)
- Blinding of data collectors and analysts will have reduced any detection bias
Weaknesses
- Four of the authors declare funding and honoraria from Deltex Medical, the manufacturer of the monitoring device, however the company had no input into the conduct or write up of the trial other than providing the equipment for free
- The definition of post-operative complications used for primary outcome assessment in this trial changed towards the end of the recruitment period
- Initially used ACS NSQIP definition, but changed to EPCO definitions
- Impact of this changed not analysed or described in the manuscript
- The authors do not describe how patients were sampled and screened for eligibility
- This is usually convenience sampling or consecutive sampling
- Screening of 496 patients from 5 hospitals over 4 years would appear to be a low rate, suggesting many eligible patients were not screened
- This may have led to a selection bias
- Were patients selected based upon favourable characteristics?
- No attempt to stratify randomisation into blocks to evenly distribute randomisation within subgroups of surgical specialty or hospital
- Block randomisation with stratification may have reduced bias by evenly allocating patients according to known confounding variables
- This trial fell significantly short of the recruitment target
- The overall power of the trial is low, increasing the risk of a false positive conclusion
- The authors point out that they did reach their target for the gastrointestinal surgery subgroup
- Given the absolute difference in the primary outcome was just 8% (much less than the estimated 19% used in the sample calculation), the actual power of the trial for this subgroup will still be less than the desired 80%
- Lack of blinding of the clinician providing intra-operative care may have introduced performance bias
- Was more attentive or selective care delivered to the intervention group consciously or unconsciously?
- 30 patients were excluded due to protocol violation or low subgroup recruitment rate
- Since the fragility index is just 3, these 30 patients could have easily changed the conclusion drawn
- This is known as attrition bias if this systematic interference has favoured one group over the other
- The authors recognise that Enhanced Recovery and reduced intra-operative fluid administration is now common place, which wasn’t the case at the time of this trial
- This reduces the external generalisability of the conclusion to today’s patients
- Similarly, epidural analgesia appears to be less common as alternative strategies are gaining popularity
- This again reduces the generalisability of this trial
- Finally, the algorithm for both groups within this trial used starch-based colloids, which are no longer available in most settings
- This led to the early termination of this trial and makes generalising the results difficult
- The authors have not postulated a credible theory to explain how GDHT has resulted in no difference in measured treatment between the groups and yet has resulted in a positive difference in the primary and some secondary outcomes
- They suggest that timing of fluid administration may be critical even if the same amount of fluid is ultimately delivered during procedures of around 3 hours, although they presented no data to support this
The Bottom Line
- The result of this trial is broadly in keeping with that of other trials such as OPTIMISE, suggesting that goal-directed haemodynamic therapy during major surgical procedures is beneficial
- However, this under-powered trial has several methodological weakness that lead me to doubt the strength of the positive conclusion, and a false positive conclusion is likely
- I will not be routinely using goal-directed haemodynamic therapy during surgery for low to moderate risk patients based on this trial alone
External Links
- [article] Effect of goal-directed haemodynamic therapy on postoperative complications in low-moderate risk surgical patients
- [further reading] OPTIMISE trial summary by TBL
- [further reading] INPRESS trial summary by TBL
- [further reading] TBL Blog: Power calculations by Imelda Galvin
Metadata
Summary author: Duncan Chambler
Summary date: 22 April 2018
Peer-review editor:Adrian Wong



