BAOIA Presentation 2018

New Evidences in Intensive Care Medicine
This editorial blog has been written to complement the short presentation delivered by Duncan Chambler at the British Association of Indian Anaesthetists (BAOIA) 2018 conference in Newcastle.
What am I hoping to deliver?
The title of the talk given to me is “New Evidences in Intensive Care Medicine”. I hope to provide a little CPD to the audience by covering a few important research findings in the field of ICM from the last 12–24 months. This is relatively easy as it’s all here, on this website.
The punch line, this early?
I’m going to start my talk by delivering the punch line early. This way, if anyone falls asleep, they’ve already taken in my key message!
- Endotracheal intubation may not be a gold standard in resuscitation
- Adrenaline remains part of Advanced Life Support
- Steroids in septic shock are justifiable
- ‘Open lung approach’ is harmful
- Fluids should be balanced
- Out of hours activity must be taken seriously
And now a disclaimer
I’m a believer in Evidence Based Medicine. I think Eminence-based or Common-sense-based medicine should be kept to a minimum and only used as a fallback when there is no relevant empirical evidence.

However, there is both science and art involved in the translation of research to clinical care. The science involves the interogation of qualitative and quantitative data to draw a conclusion based upon the Scientific Method as described by Galileo, Bacon, Newton and Einstein amongst many others in history. The art is deciding whether the conclusion is correct and applicable to the patient in question.
Therefore, throughout this presentation I am not providing facts. All I can do is provide my opinion based upon my interpretation of the published data, relevant to the sort of patient that I treat.
The context
This is an exciting time in Intensive Care Medicine. To use paraphrase Rumsfeld’s famous quote, there are known knowns, known unknowns and unknown unknowns in the provision of care to critically ill patients. The facts we consider known knowns are slowly growing in number but there are still not many. The areas in which we know we do not yet have the answers are slowly being answered by hardworking researchers and clinicians. Finally, it is our job as shop-floor clinicians to raise our hands and point out the unknown unknowns.
This is relevant to this talk because we now have some more known knowns, but most of these trials have just raised more known unknowns that need subsequent investigation. Often a trial produces more questions than answers.
I hope this talk will bring to the audience the latest theories that have moved from known unknowns to known knowns, so that our patients can recieve better care.
Meet Geoff
I plan to illustrate my key points by introducing the audience to Geoff. This is going to be a bad 20 minutes for Geoff!
Geoff is in his 60s. He lives outside Newcastle and speaks with a dialect I can’t easily understand. He’s had a cough for the past week that he can’t shift. Finally, he collapses at home and his wife calls for an ambulance.
AIRWAYS 2 and PART
When the paramedics arrive, he is unresponsive with a weak and fading pulse. They start CPR and Advanced Life Support. They realise he needs more than mask ventilation, and this raises the first clinical question.
In adult patients suffering non-traumatic out-of-hospital cardiac arrests, does the use of supraglotic airway devices compared to conventional endotracheal intubation for the initial advanced management of airways improve patient outcomes?
This clinical question has been researched by the AIRWAYS 2 trial team from Bristol and a comparable trial abbreviated to PART from the USA.
AIRWAYS 2 enrolled 9296 patients from 4 ambulance trusts across the UK and randomised them into two groups: airway management with supraglottic airway devices vs endotracheal intubation. The outcomes were similar between these groups when they looked at survival and good neurological recovery (6.4% vs 6.8%). Successful management of the airway within 2 attempts was more common in the supraglottic device group (87% vs 79%), suggesting it is easier to use in paramedic hands, but the subsequent unintended loss of airway rate was double that of the endotracheal group (10% vs 5%).
The PART trial was a similar design with 3004 patients, but the comparison was laryngeal tube vs endotracheal intubation and the outcome was just 72-hour survival. Survival was higher in the laryngeal tube group (18% vs 15%).
My interpretation of these trials is that endotracheal intubation in the community in the hands of paramedics as part of Advanced Life Support lacks a clear advantage over supraglottic devices. In my opinion, paramedic intubations will be phased out soon.
Another interesting study worth mentioning is an observational study by Lars Anderson (Anderson summary) in which tracheal intubation during in-hospital cardiac arrest was associated with worse outcomes! This points towards the need for a randomised trial to answer this known unknown.
PARAMEDIC-2
As CPR progresses, IV access is obtained and the paramedics confirm PEA. Adrenaline has been advocated for years but it’s theorised that it may be harmful, through increased cardiac oxygen demand or cerebral vasoconstriction, and this may outweigh the benefits of improved coronary perfusion.
In adult patients with out-of-hospital cardiac arrest, does the administration of adrenaline compared to placebo increase survival?
The PARAMEDIC-2 trial, run by the Warwick trial group, provides some fantastic data to explore this question. Five NHS ambulance Trusts recruited 8,103 patients to either adrenaline or placebo, with administration guided by Resusciation Council’s guidelines. Survival at 30 days was more common in the adrenaline group (3.2% vs 2.4%), with a representative Number Needed to Treat of 112, but a Fragility Index of only 6. Furthermore, the Bayesian analysis suggests that the probability of survival with a favourable neurological outcome is unlikely to be effected by administration of adrenaline.
It’s a complex paper and analysis, with various interpretations. Staying with the primary outcome, around which the trial was designed, then adrenaline administration probably improves survival and I think it should stay in the ALS guidelines. However, the secondary outcomes investigating quality of life after survival raise the possibility that adrenaline improves survival at the cost of neurological injury.
For me, the known known is that adrenaline improves survival, but this trial leave us with more known unknowns to look at in the future.
ADRENAL
Once in the hospital and stabilised, Geoff continues to deteriorate in Critical Care. The dose of noradrenaline is increasing and it appears that pneumonia is driving a process of septic shock. The clinicians consider the addition of hydrocortisone, which is theorised to supplement the exhausted or inadequate stress response and modify the excessive immune response, but possibly at the cost of unintended immune suppression.
In critically ill patients with septic shock, does hydrocortisone compared with placebo increase survival?
The ADRENAL trial attempted to definitively answer this question, and it took Dr Venkatesh years to complete this trial.
The trial team recruited and randomised 3,658 patients to either hydrocortisone (200 mg/day as continuous intravenous infusion for 7 days or until ICU discharge with no cessation tapering) or placebo.
The primary outcome, death at 90 days, was not different between the groups. The 95% Confidence Intervals suggest the true population difference lies somewhere between a 2.0% increase in death and 3.8% increase in survival. If you believe these extremes are not clinically important, then you can conclude that steroids in sepsis are not worth giving.
However, the secondary outcomes and observations by the trial team are interesting. In patients given steroids, shock resolved quicker, patients were liberated from mechanical ventilation earlier, discharged from ICU sooner and they received few blood transfusions. Some commentators have said that these are clinically important and therefore steroid administration is justified. Others have said they are underpowered repeat measurements that should only be noted as known unknowns worthy of further research.
So if you want to give steroids, you can justify giving them. If you think they are a waste of time, this trial backs you up too!
Steve Mathieu has written an extensive editorial on this topic to complement the publication of the ADRENAL trial.
ART
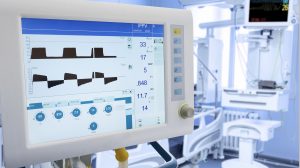
Alongside Geoff’s worsening septic shock, it becomes increasingly difficult to oxygenate him. Clinicians argue over the optimal PEEP setting and a team member suggests following the ‘Open Lung Approach’ to recruit lung units and titrations PEEP to an optimal level, but is this better than a standard ‘ARDSnet’ strategy?
In patients with moderate to severe acute respiratory distress syndrome, does the use of lung recruitment and titrationed PEEP compared to conventional low-PEEP ventilation increase survival?
The ART trial investigators recruited 1,013 patients from 120 ICUs across the globe, of which the majority had septic shock in addition to ARDS. After randomisation, half were allocated to an ‘Open Lung Approach’, which includes a lung recruitment procedure and PEEP titrations according to the best respiratory-system compliance. The remaining half were continued on conventional ventilation as previously describe by the ARDSnet KARMA trial.
The outcome was surprising. More in the novel ‘Open Lung Approach’ group died (55.3% vs 49.3%). The absolute risk difference was nearly 6% in favour of conventional ventilation, correlating with a number-needed-to-harm of 17. This outcome only just reached statistical significance according to the parameters defined by the trial team, but it’s still important.
The detail of this trial and the ‘Open Lung Approach’ strategy can probably explain this increased mortality. The recruitment procedure involved neuromuscular blockade followed by incremental PEEP up to 45 cmH2O. Yep, that’s not a typo error. In addition to this, the driving pressure (or ΔP) was set at 15 cmH2O such that the Ppeak was 60 cmH2O. It is perhaps no surprise that the authors reported frequent haemodynamic instability during these procedures.
This trial was extremely well conducted and it is reasonable to conclude that recruitment procedures and titrated PEEP performed in this way to mod-severe ARDS patients is not recommended. However, commentators have suggested that perhaps the hypothesis tested wasn’t quite right for the theory proposed, so this may not be the end of recruitment procedures and titrated PEEP in Intensive Care Medicine.
Also on this topic, the BILEVEL-APRV trial and the Reconnect trial are worth reading.
SMART
Whilst resuscitating and stabilising Geoff, he is administered several litres of crystalloid fluid. The unit pharmacist says the hospital is now stocking ‘balanced’ crystalloid in addition to regular ‘normal saline’. It’s slightly more expensive and the team aren’t sure whether it will actually make a difference.
In critically ill patients, does balanced crystalloid compared with saline increase survival, or reduce the frequency of kidney dysfunction?
The SMART trial is one of several recent trials investigating this clinical question. In 2015, the SPLIT trial concluded that a balanced crystalloid made no difference to patient outcome. The SMART trial was much, much larger and comes to a different conclusion.
This was a pragmatic, cluster-randomised, multiple-crossover trial in which ICUs randomly used one fluid or the other for all patients for a month at a time. Although this lacks some of the robustness from trials that randomise each individual patient, it allows for a more extensive trial to be effectively conducted.
In this case, 15,802 patients were included from across 5 ICUs in one large academic hospital in USA over almost 2 years. The outcome of interest was a composite of death, renal replacement therapy or persistent renal dysfunction within 30 days of admission or discharge from hospital.
The results were subtle but statistically significantly different. 14.4% suffered the adverse outcome in the balanced crystalloid group compared to 15.4% in the saline group. This absolute risk difference of just 1% equates to a number-needed-to-treat of 94 patients, which is clinically significant given the number of patients that receive fluid therapy in Intensive Care Units. No statistically significant differences were identified in individual outcome measures, so it’s hard to pick this composite outcome apart. Does saline kill, or just result in kidney injury lasting at least 30 days? The PLUS trial may help answer this known unknown.
Vollam

Finally, Geoff starts to improve. He’s weaned and liberated from mechanical ventilation and vasopressors. His delirium clears (there are plenty of known unknowns and probably plenty more unknown unknowns in that field of medicine) and he’s ready for discharge to a step-down ward. Unfortunately, beds are tight and management are asking the team to make that discharge at 1am in the night, but will that have a direct effect on Geoff’s future?
In patients discharged from a general Intensive Care Unit, is discharge ‘out-of-hours’ compared to ‘in-hours’ associated with subsequent harm?
This is highly topical, especially within the NHS where the pressure is high for all units to cope with increasing demand. The recent meta-analysis by Vollam et al attempts to address this question.
A systematic search identified 18 trials including over one million patients from multiple healthcare systems. ‘Out-of-hours’ was variably defined as starting between 4pm and 10pm, and ending between 6am and 9am.
The adjusted odds ratio of death before hospital discharge was 1.33, with a statistically significant 95% confidence interval of 1.3 to 1.36. Similar significance was found for ICU readmission rates.
There are limitations to this meta-analysis and the strength of this association may not be very high, however it adds weight to the commonly held assertion that out-of-hours discharges should be avoided.
Conclusion
So to conclude Geoff’s tale and my talk, I hold the following 6 opinions based on the evidence presented above:
- Endotracheal intubation may not be a gold standard in resuscitation
- Adrenaline remains part of Advanced Life Support
- Steroids in septic shock are justifiable
- ‘Open lung approach’ is harmful
- Fluids should be balanced
- Out of hours activity must be taken seriously
There are many unknowns remaining and I encourage all clinicians to engage in research to improve the care of our patients.
Finally, it is worth noting that nearly all the trials presented above have aimed to identify absolute differences of 1 or 2 percent for the tested intervention, whether it be a drug, fluid or procedure. Whilst these remain import trials, I believe this are tiny marginal gains in clinical care. The big differences come from the outstanding nursing care delivered every day, around the clock and around the globe. Without our nurses and allied health professionals, our patient outcomes would be considerably worse, and no new medical innovation will beat that!
Resources
The following are resources I will personally recommend to the audience for Intensive Care Medicine related education and research dissemination
Critical Care Reviews is an excellent online resource and outstanding annual conference
http://www.criticalcarereview.com
Life in the Fast Lane has a wealth of resources applicable to every busy Intensive Care Medicine doctor
Http://www.lifeinthefastlane.com